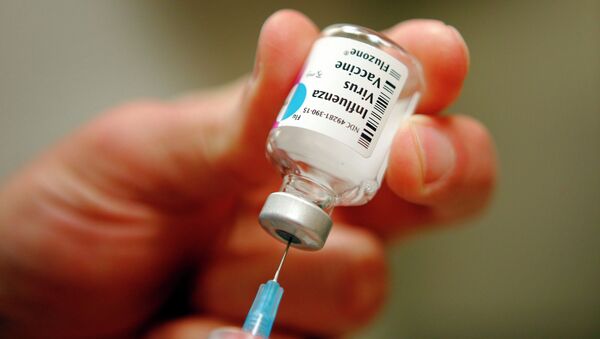
Barney Graham, NIAID's deputy director of vaccine research, claimed that have recently been provided with the tools to "design things at atomic resolution." At present, vaccines target the "head" of the influenza virus, which changes between strains. The "stem" of the virus is unchanging, so a vaccine that targets that portion only would be able to prevent every strain of influenza, instead of just the two or three that seasonal vaccines are intended to treat. The "tail" is difficult to target, but molecular engineering could be the path to doing so.
"[A universal vaccine] would be the single most important thing we can do in public health today," said Michael Osterholm, director of the Center for Infectious Disease Research and Policy. The Centers for Disease Control and Prevention (CDC) reported that 40 percent of Americans have received their flu shot this year, but officials believe that they could greatly increase the number of protected individuals if a vaccine was only needed once every five or ten years.
A universal vaccine would also be less expensive to manufacture and distribute. The flu vaccine industry has exploded to a four-billion-dollar global business in 2015, after the CDC expanded its recommendation of annual vaccines to every American older than 6 months in 2010. Even if a universal vaccine was more expensive per unit, it would likely cost less overall, as manufacturers would make less.
Officials also offer that a universal vaccine would be more reliable. At present, health officials must make an educated guess as to what will be the most dangerous and virulent strains of influenza in nine months, to give manufacturers time to produce the correct vaccine. "Each year we could go after people who hadn't been vaccinated before. It could be a year-long, daily vaccination activity, not just focused in the fall," said William Schaffner, medical director of the National Foundation for Infectious Diseases.
Annual cases of influenza in the United States vary greatly from year to year, but typically fall within the range of 16-64 million people. Most of those cases are minor, but typically around 23-36,000 Americans die from the disease, or its complications. The greatest incidence of influenza in modern history was the 1918 Spanish Flu outbreak, which left 50-100 million dead worldwide. While unlikely to recur, experts believe a universal vaccine would reduce the chances of such an outbreak even further.
The CDC estimates that the vaccine prevents 5 million flu illnesses and 71,000 hospital visits. It is only about 50-60 percent effective most years, but saves thousands from hospitalization or death.