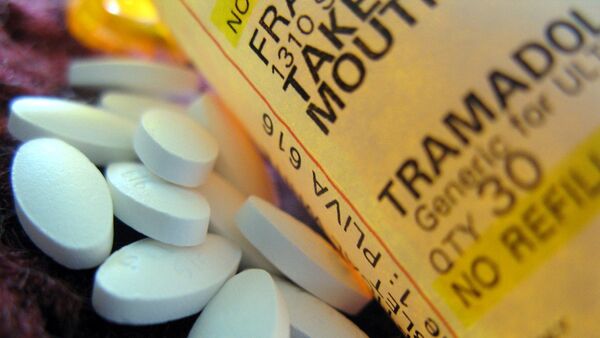
Doctors decided to prescribe him a tramadol based treatment.
“Tramadol is a common treatment for back pain. They gave it to me again to cure the inflammation of my heel tendon, as I am allergic to anti-inflammatory drugs, and once again to relieve pain when I had Lyme,” the athlete says. “For several years, I took fairly small doses several times a week, but not regularly. When I suffered from Lyme disease, I was prescribed the maximum dosage of tramadol, 400 mg per day.”

No one ever warned him about the possibility of addiction. Sometime later, the effect of tramadol started becoming weaker and weaker and Chris began increasing the dose. He quickly developed an addiction. The father of two lost his family because of his addiction. His wife couldn’t live with a drug addict.
Tramadol withdrawal syndromes can be similar to heroin withdrawal syndromes – depression, anxiety, sweating, vomiting, palpitations, inability to sleep, vivid dreams, tremors, mood swings...
“Last week was the hell of the French medical system. I’m fine; I’ll leave the hospital soon. The first part of the treatment — the withdrawal from tramadol — was quite successful. Unfortunately, the second part was not, since the combination of antidepressants and other drugs they gave me infuriated me, I lost the sense of who I was or where I was, I was running naked down the street,” Chris wrote from the rehab clinic.
According to a new report by the French National Agency for Medicines and Health Products Safety (ANSM – Agence Nationale de Sécurité du Medicine and des Produits de santé), in recent years, France has experienced an increase in the consumption of opioid analgesics. One of the most consumed drugs is tramadol, an opioid analgesic of moderate strength. Between 2006 and 2017, tramadol consumption increased by 68%.
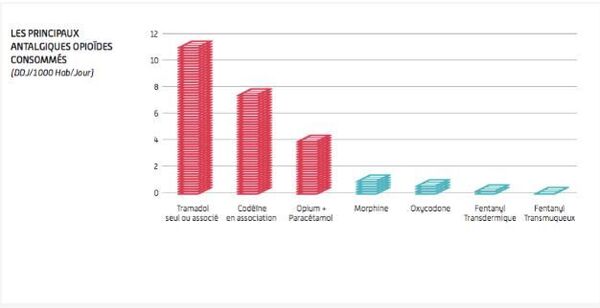
Chris was lucky to wean off his addiction. Those who lost their loved ones because of these prescription drugs tried to sound the alarm in French society, but every year there are more and more deaths caused by opioids.
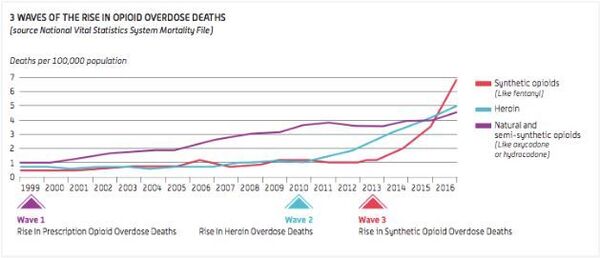
“Currently in France, there is a serious risk of an opioid crisis. An increase of hospitalisations due to overdoses of potent opioids as well as deaths for the same reason is envisaged. We have to act urgently to avoid a real crisis. Using the examples of the United States and Canada, we realised that it’s very difficult to put an end to such a crisis,” Nicolas Authier, an addiction psychiatrist from the ANSM, says. “In France, tramadol is the most prescribed drug. Up to 5.8 million people take this drug annually. Of course, the vast majority of overdoses and deaths are associated with tramadol,” the professor warns.
These painkillers work very well for pain therapy. But patients taking these drugs are at risk of addiction. ANSM experts recall that more than 50 per cent of tramadol withdrawal symptoms occur after therapeutic doses, sometimes even for very short periods of time; this is what practitioners who prescribe such drugs don’t mention to their patients.
“I started taking pills before workouts because I felt a boost and it helped me at work. It was at that moment that I realised I was experiencing some kind of psychological dependence on that drug. At that time I must have taken it every day. I had panic attacks when I didn’t have the right dose with me. It was no longer about pain,” Chris explains.
For 4 years he had been suffering from the addiction. He himself told the doctor about this and was referred to the addictology department. “I was treated together with heroin addicts. I was the only patient who was being treated for tramadol addiction. At that time it was something new, while today it is becoming more and more common. I suffered just as much as the morphine or heroin addicts suffered,” the man says.
According to Barbara Szelesky, a practising physician at the Center for Pain Intensity and Pain Therapy at the Foch Hospital in Suresnes (CETD – Center D'Evaluation et de Traitement de la Douleur de l'Hôpital Foch de Suresnes), “unfortunately, tramadol has a very large abuse potential,” and initially doctors “didn’t particularly realise this.” The expert thinks that the high frequency of consumption of tramadol is explained by the withdrawal of Di-Antalvic from the European market. The substance was banned in 2011 on the recommendation of the European Medicines Agency (EMA). At one time, experts from the French Agency for the Control of the Sanitary Safety of Medical Products (AFSSAPS - Agence Nationale de Sécurité du Médicament et des Produits de Santé) that became ANSM in 2012, expressed bewilderment about this decision. At that time, the Head of the Agency shared his concerns about the risk of the “large-scale replacement of prescribed drugs with tramadol,” which would entail “negative consequences for public health”.
Another opioid analgesic that is worth mentioning is oxycodone which is classified as a potent opioid. According to ANSM, in France, from 2006 to 2017, its consumption increased by 738%. Since oxycodone has a powerful analgesic effect, its use is controlled better than the use of other drugs. “I personally prescribe oxycodone only for chronic cancer pain,” Barbara Szelesky explains.
According to a new Grand View Research, Inc. report, in 2018, the global opioid market was estimated at $25.4 billion.
North America leads the market with a 55.5% share of the revenue.
Europe is the second largest regional market. The UK, Germany, France and Spain show the highest opioid turnover in the region. Consequently, these are the same countries that rank first in the list of opioid users on the continent.
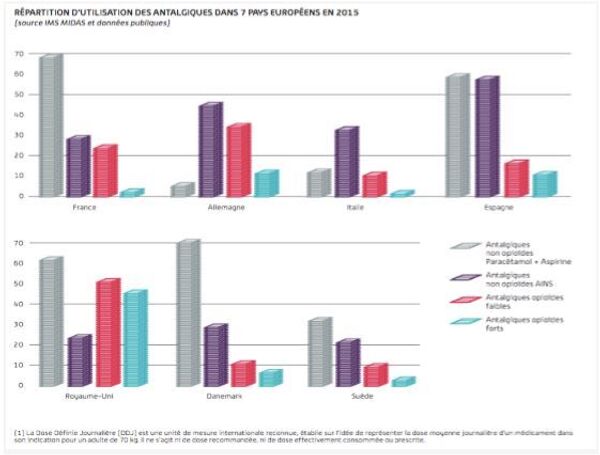
EMA and the Pharmaceutical Industry.
The European Medicines Agency was founded in 1995. The Agency’s main task is to protect human and animal health.
The pharmaceutical industry is one of the main stakeholders of the EMA.
It’s worth noting that on the agency’s website there is a table with tariffs for permission to advertise and sell drugs. The starting rate for obtaining such certification is €291,800. Additional paid services are also offered, such as extending the term of an existing permit.
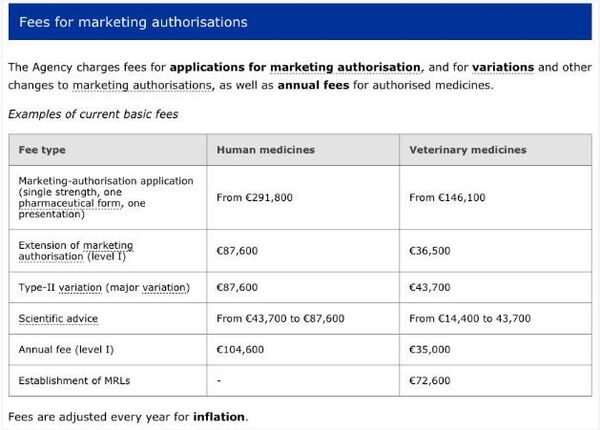
Since the EMA provides paid services, can there be a conflict of interest between the agency and pharmaceutical manufacturers? In an open letter on June 2010, members of the International Society of Drugs Bulletin (ISDB) sharply criticised the “failure of simple solutions to avoid conflicts of interest at the level of the executive board” of the EMA. In this regard, the authors of the 2012 EU Accounts Chamber Report on the resolution of conflicts of interest within EU agencies drew a frightening picture. Regarding the EMA, they say that “owning financial assets --- and patents is prohibited for agents, but not their family members.”
In 2011, in response to growing citizen demand for a better definition of relations between doctors and pharmaceutical manufacturers, a bill was adopted to strengthen the control over the sanitary safety of medical products. The law provides for the publication of lists of people or organisations which healthcare manufacturers have signed agreements with or whom they have provided remuneration to. In 2014, the Transparency-Healthcare website (Transparence-Santé) was created to post any information that could provide information about “each type of overlapping interests”.
In the reward document, which is more than 2 million lines long, Sanofi (one of the tramadol manufacturers) is mentioned 33,665 times. This French multinational pharmaceutical company is the fifth largest in the world, in terms of prescription drug sales since 2013.
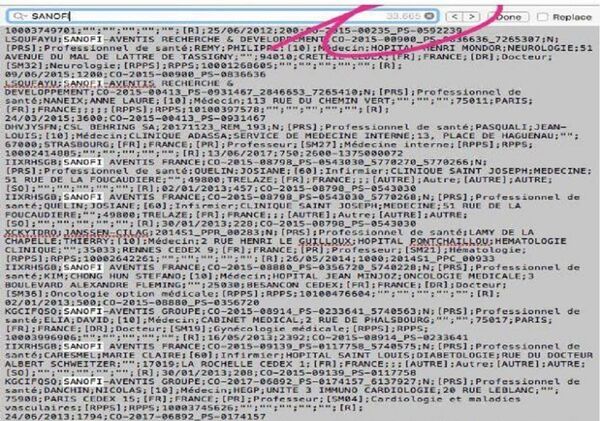
Many questions arose regarding the reliability of this resource. Observers noticed some errors, omissions, and the lack of details... The transfer of several million euros is mentioned; with no indication of on what basis this money was received.
The Regards Citoyens Association conducted an investigation into the transfer of funds from pharmaceutical manufacturers to doctors and clinics. In 2015, the Association published a list of the most “generous” donors. Sanofi was among the top 15 companies on the list.
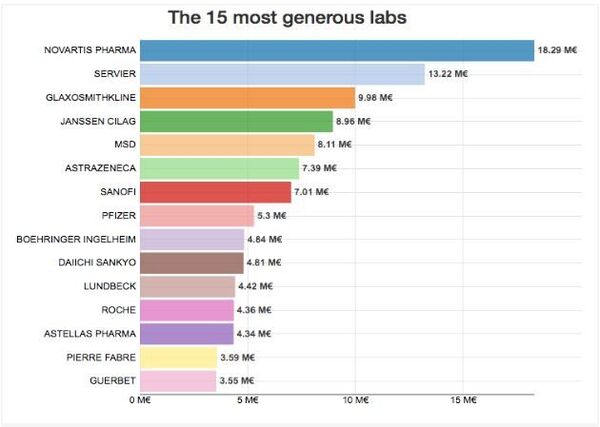
According to Professor Authier, “it goes without saying that the goal of pharmaceutical manufacturers is to sell medical products to doctors. And this is problematic when it comes to drugs that cause greater or lesser degrees of addiction. One would expect firms to have a higher level of responsibility and more ethical behaviour. They have to take responsibility for the role they play in the opioid crisis.”
Of course, all opioid drugs are prescribed exclusively by doctors. In recent years, significant progress has been made in the use of strong opioids for cancer pain.
Doctors don’t have the right to prescribe tramadol for more than one year. Pharmacists have the right to issue tramadol for a maximum of 28 days. The duration of oxycodone treatment cannot exceed 28 days, and doctors are not allowed to renew prescriptions.
ANSM experts emphasise that only thanks to these tough measures has France avoided a large-scale crisis similar to that, which the US is experiencing. From 1999 to 2017, nearly 218 thousand people died from overdoses associated with prescription opioids. The prescription opioid overdose mortality was five times higher than in 1999. In October 2017, as a result of the opioid crisis, a state of emergency was declared in the field of health care.
The ANSM report, however, indicates that the number of abuse cases for opioid analgesics in France has more than doubled between 2006 and 2015.
Chris thinks it’s very easy to get tramadol in France: “When I went to my doctor, he asked me how much I used. If I said [I used] 400 mg, he gave me that dose. He never thought that maybe I should stop using this drug. In England, I couldn’t have gotten tramadol so easily. They would just give you enough drugs for a week and tell you to come back to check how you were doing. Here they gave me prescriptions for three months.”
Marion Bobillot, a student at the Nursing Institute at the St. Louis Hospital in Paris (IFSI - Institut de Formation en Soins Infirmiers de l'Hôpital Saint Louis), explained what students are taught about cases in which opioids should be prescribed: “Analgesics are given gradually, depending on pain intensity on a scale from 0 to 10. The first degree is from 1 to 4; the second is from 4 to 6 or 7; from 7 to 10 is the third degree, severe pain. Tramadol is prescribed when a patient suffers from second-degree pain.” The student knows firsthand how tramadol acts. “Once, my dentist prescribed me tramadol. I remember it’s a very strong drug, I was a bit high when I took it.”
The American experience shows that in many cases opioids lead to heroin addiction – according to reports, about 80 per cent of heroin users said they used prescription opioids before heroin, the drugs which are currently the main cause of overdoses in Europe.
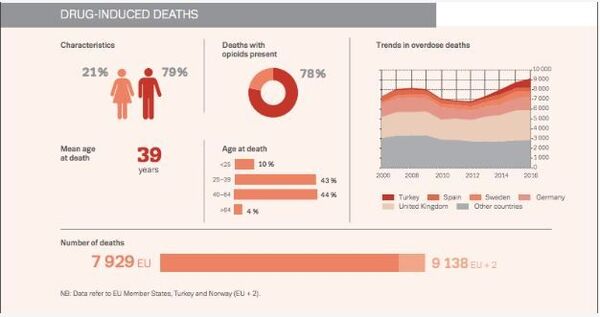
The data on the growing number of deaths associated with the consumption of opioids is also evidence of a worsening situation in France. According to the ANSM, we are talking about “at least 4 incidents a week.” In 2015, almost 10 million patients (approximately 17% of the country’s population) were prescribed opioid analgesics. More than 85% of opioids are prescribed by a general practitioner. Next on the list are dentists, rheumatologists and orthopaedic surgeons.
“The prescribed consumption of opioid analgesics doesn’t necessarily entail addiction,” Patrick Bartel, a retired general practitioner, emphasises. But those who become addicted to these drugs find it difficult to find support in the healthcare system: “This is a vicious circle,” Chris says, “when you find yourself there, doctors don't find it so easy to stop giving it to you. I admitted to myself that I was addicted. It was hard for me to say that I had become a drug addict! It was not the doctor that diagnosed my addiction, it was me. And nobody else!”
Professor Benjamin, an addiction psychiatrist at the Paul Brouss hospital in Villejuif and President of the French Federation of Addictions, believes that informing patients about the risk of addiction to analgesics and monitoring patients is “not at the best level”. He adds that “first of all, it’s necessary to conduct a new assessment of existing drugs,” and “it’s also necessary to inform the doctors about alternative methods of pain management”. According to Professor Benjamin, in most cases, instead of analgesics, patients can be offered massage, psychotherapy, relaxation, or sports.
“In France, for 2 years now we have seen the same thing happening that is happening in the US,” Professor Authier says with fear, “we are talking about this more and more. But apparently, this is not yet optimal.”
Chris insists that if nothing changes in the near future, more and more people will suffer from severe addictions to tramadol.
“Tramadol is a completely new danger. Ordinary general practitioners don’t know how addictive it is. Since this is a synthetic opioid, it was perceived not to have the effects attributed to natural opiates, but that was completely wrong. Getting off of tramadol is just as bad as giving up some of the more illicit drugs.”