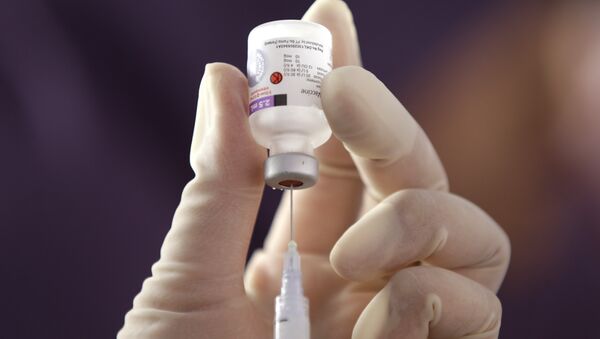
However, many are still sceptical about the vaccine, with some even considering it to be a morally unsound programme.
Dr Sue Sherman, a senior lecturer in psychology at Keele University, underlined the success of the HPV vaccination for girls and explained the reason for the delay of the inoculation for boys.
SPUTNIK: Since 2008, girls have been offered the HPV vaccine between the ages of 12 and 13. Can you tell me a little bit about the impact that's had?
Sue Sherman: There was some research published a couple of months ago which demonstrated that the vaccine has been very successful, it's reduced the incidence of HPV infections in young women and also in the number of cases of precancerous cell changes that we're seeing in young women.
SPUTNIK: Why has it taken so long for boys to be considered for this inoculation?
Sue Sherman: There's a variety of reasons why boys weren't vaccinated, or why the vaccination programme wasn't introduced to the boys at the same time it was for girls. Firstly, that was 11 years ago, and back then the evidence about the association of HPV with other cancers - cancers that affect males - wasn't as well established as it is now. Secondly, there's always been an argument about something called herd immunity, the idea being that if you vaccinate enough girls, that boys will be protected. Of course, there's always also the cost-effectiveness argument. So it wasn't clear, that there was going to be sufficient cost savings to make it an effective addition to the vaccination programme in the UK.
SPUTNIK: At the moment, this has been offered to young boys; however, with young men who miss out on the vaccine, is there a benefit in them getting the inoculation as well?
Sue Sherman: What the NHS is saying at the moment is that if young men aren't vaccinated, either because they miss it or because they're not in the right age group to get vaccinated, then they should still benefit from the herd immunity that I mentioned earlier. This is the idea that if the girls are protected against the virus, then the virus isn't in circulation. For those men, such as men who have sex with men, up to the age of 45, they're able to still get the vaccine free from sexual health clinics and HIV clinics.
SPUTNIK: Are there any side effects of the HPV vaccine that people should be concerned about?
Sue Sherman: There can be some local side effects, a little pain at the injection site and so on. But back in 2017, the World Health Organisation issued a statement which directly addresses the safety concerns associated with the vaccine. As of 2017, there had been 270 million doses administered worldwide and large scale epidemiological studies revealed that there was no difference between the vaccinated and unvaccinated populations in the rates of serious adverse effects.
SPUTNIK: What could you say so that none of our listeners are concerned that the HPV vaccine encourages riskier sexual behaviour among people who have received it?
Sue Sherman: This is a common concern amongst parents. However, there has been research done; there was research done after a few years into the girls' programme. What they found was that actually it doesn't increase promiscuity and actually, in many cases, it makes girls more aware of their health and actually enables them to make better choices and be more aware and be more safety-conscious.
The views and opinions expressed in this article are solely those of Sue Sherman and do not necessarily reflect Sputnik's position.