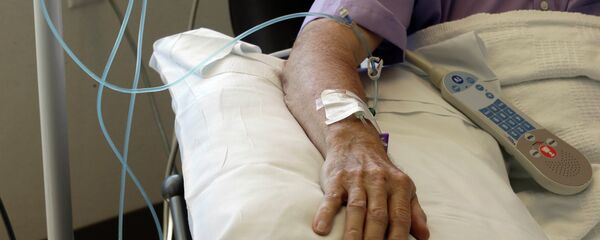
A nondescript New York medical clinic sees 65 patients every week who suffer from America’s most common mental illness, depression, where they undergo a 45-minute treatment: the intravenous infusion of ketamine. The price tag per session is $525.
Brooks was driven to found the treatment center after he lost his son, a drug addict who committed suicide in 1991 after losing his battle with depression. Some twenty years after Brooks started research on ketamine, he opened a detox center for opiate addicts, prompting calls from psychiatrists who wanted to know whether he could treat suicidal patients with ketamine as well.
“For ketamine to work there needs to be some preexisting brain damage caused by post-traumatic stress,“ Brooks commented, stressing that patients can come to his office without a prescription.
Although New York state law doesn’t prohibit administering ketamine for non-approved uses, the US Food and Drug Administration hasn’t confirmed the use of the hallucinogen as a safe treatment for mental disorders, despite a number of medical studies indicating that severe depression had been eliminated by the drug.
Some 70 percent of his patients have registered some improvement; they are administered a lower dose of ketamine than that commonly preferred among club revelers.
Ketamine was first developed in 1962 and is still used during numerous operations and for pain control.
In 1999 the US Drug Enforcement Administration ruled that ketamine was a Schedule III controlled substance, meaning that the drug has a currently accepted medical use in treatment in the United States, but that abuse of the hallucinogen may lead to moderate or low physical dependence or high psychological dependence.
The first attempts to use ketamine to treat depression were made by Yale-based professors, who conducted researcher on the drug, which was known to block some glutamate receptors in the brain. Some years later, 70 percent of the test subjects reported that their depression had gone into remission, surprising skeptics who believed the drug only had short-term effects. Since then, dozens of studies have confirmed ketamine’s long-lasting positive changes in the brain.
“It’s settled—to my mind beyond a shadow of a doubt—that ketamine has a powerful antidepressant effect for as many as 50 percent of people where other medications haven’t been helpful,” says Michael Thase, a psychiatry professor from the University of Pennsylvania, who has followed the first ketamine tests.
Whether the FDA approves ketamine for the treatment of depression depends on a complex series of clinical tests. Meanwhile, Big Pharma hopes to develop their own, more expensive drugs that mimic the effects of ketamine, as they fear that the multi-billion dollar anti-depressant industry will lose profits to a drug with dubious associations which can be manufactured freely, as it has been around for over 50 years. “You can get a few years of exclusivity for a new use, but generally you need more than a few years to recoup the research and development costs of bringing a drug to market,” Thase said.
Brooks is always busy at work, as long as there are people arriving at his office seeking a treatment. “No one gets turned away, especially if they’re suicidal,” Brooks says. “It just gets more and more personal. I kind of see my son’s face in everyone who comes in.”